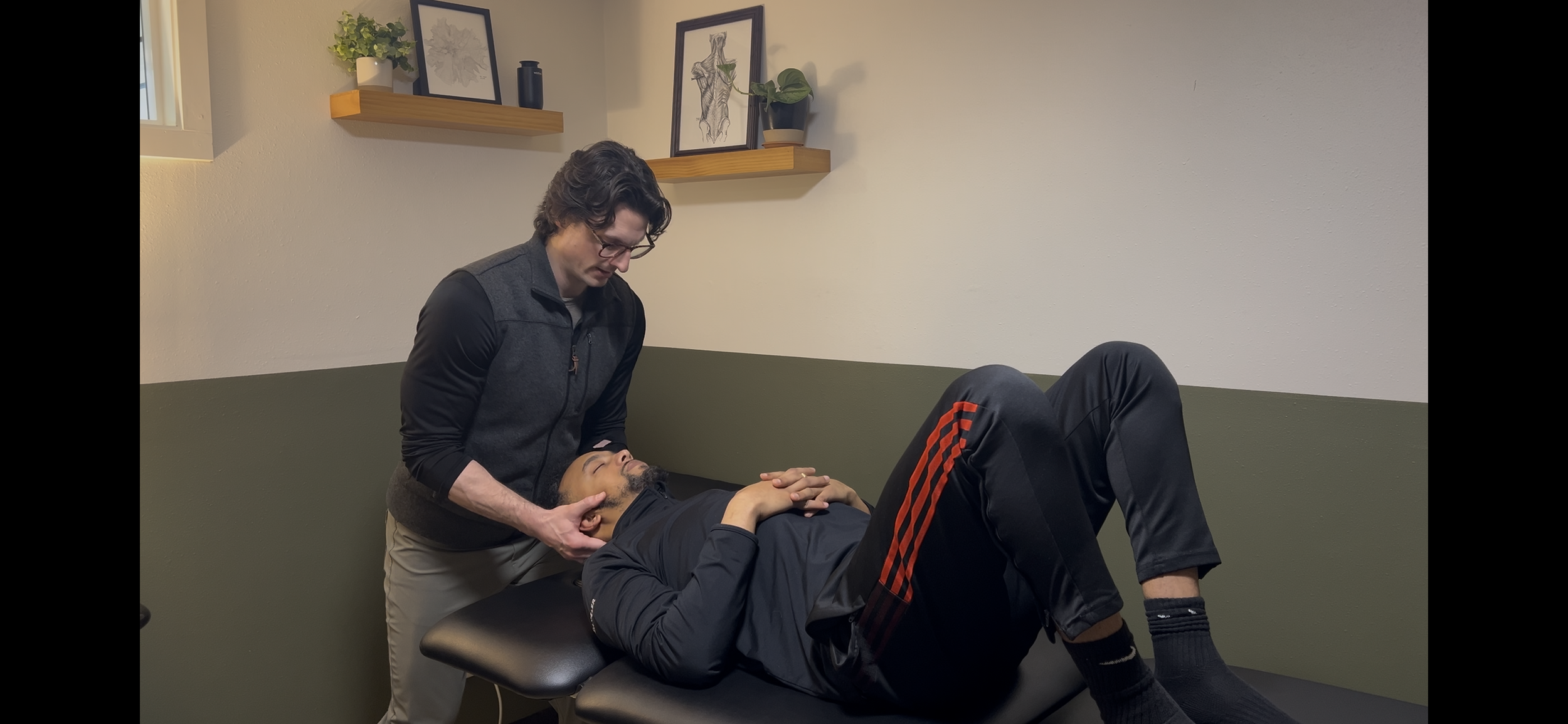
Why You Keep Getting Tension Headaches (And Why the Answer Might Be in Your Neck)
You know the routine. The headache creeps in around 2pm. You drink some water, take ibuprofen, maybe stretch your neck against your chair. It backs off. Then tomorrow, or the day after, it's back.
If that cycle sounds familiar, here's something worth knowing: the headache you've been calling a tension headache might not be starting in your head at all. For a lot of desk workers and screen-heavy professionals, the source is the cervical spine, and that distinction changes everything about how you treat it. It's a common patterns we see in the clinic, especially this time of year when screen time spikes, stress compounds, and the usual coping strategies stop working.
What's Actually Happening When You Get a "Tension" Headache
Tension-type headache is the most common headache type in the world, affecting around 38% of the global population. But "tension headache" has become a catch-all term for any headache that isn't a migraine or cluster, and that's where things get muddled.
A separate category, cervicogenic headache, originates from the structures of the cervical spine. The pain is referred upward from the neck into the head, sometimes reaching the forehead, temples, or behind the eyes. It can feel nearly identical to a tension headache from the inside. The difference is where it's coming from and, critically, what can actually fix it.
Estimates suggest cervicogenic headache accounts for somewhere between 15 and 20 percent of all headache disorders. In people who spend their days at a desk or on a screen, that number likely skews higher.
Why Desk Work Sets This Up So Well
Prolonged sitting creates a specific set of conditions in your cervical spine. Forward head posture, even subtle forward head posture, increases the load on the muscles and joints at the back of the neck. Sustained positions without movement cause muscle guarding and joint stiffness. Over time, that tension builds a pattern that reliably refers pain upward.
Spring makes this worse for a specific combination of reasons. Allergy season brings more sinus pressure and facial tension. End-of-quarter deadlines mean more hours in front of a screen and less time moving. Stress causes people to unconsciously brace their shoulders and jaw, loading the upper trapezius and suboccipital muscles directly involved in cervicogenic symptoms. It's a convergence of triggers that tends to hit people in March and April harder than almost any other time of year.
If the desk setup itself is part of the problem, Fix Desk-Related Neck Pain: Ergonomic Tips from a Physical Therapist covers the specific changes that reduce cervical load during a workday.
A 2024 randomized study looking specifically at office workers found that combining physical therapy with workstation ergonomics changes produced roughly 53% improvement in cervicogenic headache frequency over six months. That's not a minor finding. It suggests that for people in desk-heavy jobs, the right targeted approach produces meaningful, measurable results.
How to Tell If Your Headache Is Coming from Your Neck
You can't fully diagnose this on your own, and it's worth getting evaluated by a physical therapist who can do a proper cervical assessment. But some patterns point toward a cervicogenic source.
The pain tends to start at the base of the skull or upper neck before spreading upward. It often gets worse with sustained neck positions or specific neck movements. It may be primarily one-sided. When someone presses on the joints at the top of your cervical spine, it reproduces or changes your headache. You may have neck stiffness alongside the headache, not just after it.
Migraine and tension-type headache can overlap with some of these features, which is why evaluation matters. But if several of these patterns fit your experience, the neck deserves a closer look.
What Most People Try First
Ibuprofen. More water. A better pillow. Stretching the neck against the back of the chair. These aren't wrong, exactly. They just address the output, not the source.
Pain medication quiets the signal. Hydration matters. Stretching provides temporary relief to the muscles. None of them address what's happening at the cervical joints or in the deep neck muscles that are actually generating the problem. So the headaches come back, on schedule, because the underlying issue hasn't changed.
What PT Does for Cervicogenic Headache
This is where physical therapy tends to surprise people. Most patients don't think of a physical therapist as the person to call for a headache. The research suggests they probably should.
The hands-on work is where results tend to come fastest. Two primary manual therapy approaches have strong evidence for cervicogenic headache: joint mobilization and spinal manipulation. Both target the upper cervical spine, specifically the joints at C1 and C2 where the nerves that refer pain into the head originate. A 2023 systematic review found that manual therapy significantly reduces how often cervicogenic headaches occur, and most patients notice that reduction within the first one to three sessions.
Spinal Manipulation: What It Is and Who Performs It
Spinal manipulation for the cervical spine is something most people associate with chiropractors. Fewer people realize that physical therapists with advanced manual therapy training perform cervical manipulation as part of evidence-based care for conditions exactly like this.
The technique involves a precise, controlled thrust applied to a specific spinal segment, typically lasting less than a second. The goal is to restore joint mobility, reduce pain, and interrupt the referral pattern that's been generating the headaches. When it's the right tool for the right patient, it can produce a notable shift in symptoms quickly.
Safety is worth addressing directly. A thorough intake screens for contraindications before any manual techniques are applied, including a neurovascular screen and review of your history. For the appropriate patient, the risk profile of cervical manipulation is low, and the evidence for its effectiveness in cervicogenic headache is well-established. If manipulation isn't indicated for you, or you'd prefer to avoid it, joint mobilization achieves similar outcomes through gentler, non-thrust techniques and is equally well-supported in the research.
The rest of the treatment picture builds around the manual work. Deep neck flexor strengthening addresses the muscle weakness that allows forward head posture to develop in the first place. Postural retraining helps change the sustained positions that keep loading the same structures day after day. Myofascial Decompression (Cupping) and IASTM (Instrument Assisted Soft Tissue Mobilization) address the muscular component alongside the joint work. For more on how we approach the cervical spine as a whole, see our Neck Pain treatment page.
The goal isn't just to make the current headache go away. It's to make the next one less likely.
What to Expect at Your First Visit
A cervical assessment doesn't feel like going to a neurologist or getting imaging. Your physical therapist will ask about your headache pattern, look at how your neck moves, and test the specific joints and muscles involved. Manual treatment often starts in the first session, not weeks into a long intake process.
Most people leave their first visit with a clearer picture of what's actually driving their headaches and at least some reduction in symptoms. That combination of understanding and early relief is what makes this approach different from managing pain and hoping it improves.
If you're in Happy Valley, Clackamas, or the surrounding area and you've been stuck in the ibuprofen cycle, it's worth finding out whether your neck is the real problem. In Oregon, you don't need a referral to see a physical therapist directly. Book online at HERE or call or text 503-567-4035.
Frequently Asked Questions
Can PT really help headaches, or is that just for neck and back pain?
Physical therapy is one of the most well-supported treatments specifically for cervicogenic headache. The evidence is clearest for manual therapy directed at the upper cervical spine. If your headaches have a neck component, PT should be in the conversation. You can also read more about how we approach headache care on our Headache Treatment page.
How do I know if my headache is cervicogenic or just a regular tension headache?
A physical therapist can assess this in one visit. Signs that point toward cervicogenic origin include pain starting at the base of the skull, headaches that worsen with neck movement or sustained positions, and tenderness at the upper cervical joints that reproduces your symptoms.
How quickly can PT help?
Many patients with cervicogenic headache notice meaningful relief within the first one to three sessions. Long-term improvement typically involves several weeks of care combining manual treatment and targeted exercise.
Do I need a referral to see a physical therapist in Oregon?
No. Oregon is a direct access state, which means you can schedule with a physical therapist directly without a physician referral.
Will my insurance cover PT for headaches?
Timber and Iron Physical Therapy is in-network with First Choice Health, Regence Blue Cross Blue Shield, and MODA Health, and accepts motor vehicle accident and workers' compensation claims. Contact us to verify your specific benefits before your first visit.
This content is for educational purposes only and does not constitute medical advice. For guidance specific to your situation, schedule a consultation with a physical therapist at Timber and Iron Physical Therapy.