Knee Pain Treatment in Happy Valley, OR
Your knee hurts. You've probably already Googled it, maybe seen a doctor, possibly heard the word 'arthritis' or seen an MRI report full of words that sound worse than they are. Here's what the research actually shows: the findings on imaging — the degeneration, the meniscus changes, the wear — are present in almost everybody. They don't reliably predict pain, and they don't reliably predict how well you'll recover.
What does predict recovery is how you load the knee, how strong the surrounding hip and quad musculature is, and whether you have a progressive plan that keeps you moving while the irritation settles. That's what PT is for.
What the Research Says
MRI studies find significant abnormalities in 97% of symptom-free knees — degeneration, meniscal changes, bone marrow lesions — in people with zero pain (Horga et al., Skeletal Radiology, 2020)
The American Academy of Orthopaedic Surgeons lists strengthening, aerobic exercise, and physical activity as first-line treatments for knee osteoarthritis — ahead of surgery and injections
Exercise-based rehab consistently matches or outperforms surgery for meniscal tears and mild-to-moderate OA in study after study — the knee responds to load, not rest
What Causes Knee Pain?
Knee pain rarely has a single cause. More often it's a combination of load, movement patterns, and tissue capacity that's gotten out of balance. The most common presentations:
Patellofemoral pain (runner's knee) — irritation under or around the kneecap, usually from a quad or hip strength imbalance
IT band syndrome — lateral knee pain common in runners and cyclists, driven by hip and glute loading patterns
Patellar tendinopathy — pain at the front of the knee below the kneecap, from repetitive loading in jumping or heavy squatting
Meniscal irritation — often not the tear itself but the way the knee is loading around it
Knee osteoarthritis — more manageable than most people expect with the right progressive exercise program
ACL or post-surgical rehab — returning to sport or activity after repair requires careful, progressive loading that most post-op protocols underdeliver on
General deconditioning — knees that have been offloaded due to fear or pain often hurt more, not less, because the surrounding muscles lose their capacity to absorb force
If your knee pain is worst on stairs — going up or down — the pattern usually points to quad strength and patellar tracking. Our post Knee Pain Going Up Stairs: Causes and Fixes from a Physical Therapist breaks down exactly what's driving it and what you can do about it.
Timber and Iron's Approach to Knee Pain
Ryan's assessment starts with how the whole lower chain moves — the hip, the knee, and the ankle all influence each other. Pain at the knee is often a symptom of something that's breaking down upstream at the hip or downstream at the foot. Treating the knee in isolation misses half the picture.
Every appointment is 60 minutes, one-on-one. There's no rotating through exercises in a corner while waiting for the next technician. The plan is built around what you're trying to get back to — whether that's squatting heavy, finishing a race, hiking the Gorge trails, or just going down stairs without bracing yourself.
Treatment options we use for knee pain:
Spinal and joint mobilization — addressing any hip, lumbar, or ankle restriction contributing to knee load
IASTM (Instrument Assisted Soft Tissue Mobilization) — targeted work on the IT band, quad tendon, patellar tendon, and surrounding tissue
Soft Tissue Mobilization — hands-on release of the quad, TFL, calf, and hip flexors
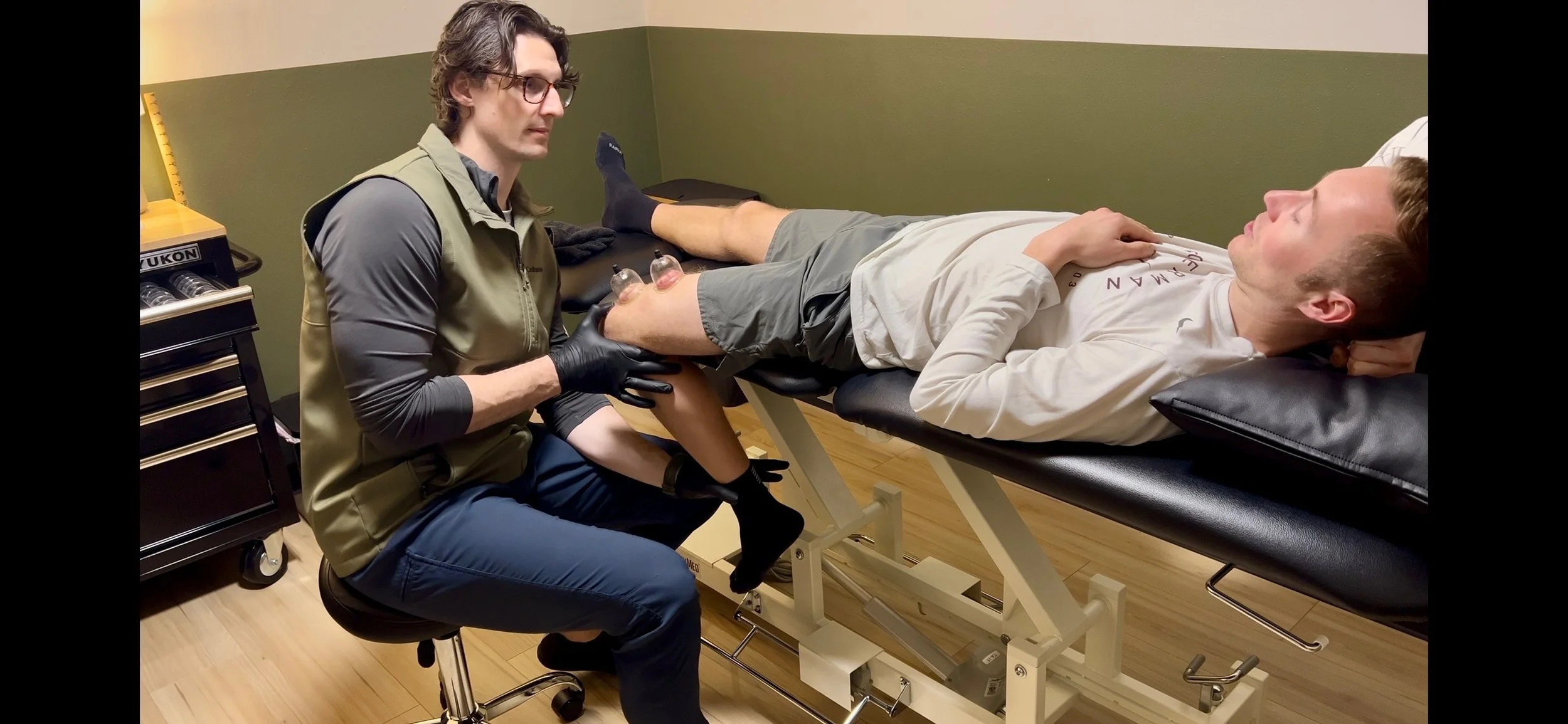
Myofascial Decompression (Cupping) — decompress the posterior knee and lateral quad
Blood Flow Restriction Training (BFR) — rebuild quad and calf strength at low loads; especially valuable post-surgically or when heavy loading is still too painful
Targeted Strength and Conditioning — progressive hip, quad, and single-leg loading built around your goals and current capacity


What to Expect at Your First Appointment
The first visit includes a full movement assessment — how you squat, step, and load through a single leg — plus hands-on evaluation of the knee, hip, and lower chain. Most patients leave with a clearer explanation of what's actually happening than they've gotten from prior appointments, plus two or three exercises to start building capacity right away.
If you've been managing knee pain for months or years and feel like you've tried everything, that's often because the approach has focused on the symptom rather than the movement problem behind it. The goal isn't to get you out of pain temporarily — it's to build the knee's capacity so the pain doesn't come back.
No referral needed — Oregon is a direct access state. Book directly online.
Common Questions About Knee Pain
My doctor said I have bone-on-bone arthritis. Is PT still an option?
Yes — and it's usually the best first option. 'Bone-on-bone' is a phrase that sounds like an endpoint, but the research doesn't support that. Cartilage health responds to load, and strengthening the muscles around the joint changes how force is distributed across it. Most people with significant arthritis findings on imaging do very well with a progressive exercise program. Ryan will tell you honestly if your situation is one where surgical consultation makes sense.
I had a meniscus tear. Do I need surgery before starting PT?
Not necessarily. For most non-traumatic and degenerative meniscal tears, the research shows PT outcomes match surgery — and without the recovery time. For acute traumatic tears or tears with mechanical symptoms like locking, surgical consultation is appropriate. If you're weighing the decision, Ryan can walk you through what the evidence says for your specific presentation. For a sense of what surgical rehab looks like when it is the right call, our post on ACL Injury Recovery Timeline: What to Expect at Every Stage covers how PT fits into post-op care.
Will exercise make my knee worse?
The fear that movement will cause more damage is one of the biggest barriers to recovery — and it's almost never accurate. Joints need load to stay healthy. The key is progressive loading: starting at a level your knee can handle and building systematically from there. Avoiding movement typically makes things worse over time, not better. For more on how active adults navigate pain and tissue changes as they age, our post on Staying Active in Your 40s and 50s: A Physical Therapist's Guide to Lifelong Movement is worth a read.
How long does knee PT take?
It depends on how long the problem has been building and what's driving it. Acute presentations like a recent strain or post-surgical rehab have fairly predictable timelines — 8 to 16 sessions with consistent home exercise is typical. Chronic patterns that have been developing for years take longer to unwind. Most patients see meaningful improvement in the first 4 to 6 sessions, which is usually enough to know the approach is working.
Knee pain doesn't mean bad knees. Book directly HERE — no referral needed in Oregon.
